World Malaria Day 2022: Placing adaptation and responsiveness at the core of community-delivered models: Zero malaria is possible
This is a guest post from Malaria Consortium, an international non-profit organisation specialising in the comprehensive control of malaria and other communicable diseases – particularly those affecting children under five.

Today marks the 16th annual World Malaria Day and provides an opportunity for the global community to reflect not only on the progress that’s been made but what more still needs to be done. As long as malaria exists, it will be a chronic engine of poverty and inequality, burdening the poorest and most vulnerable communities, almost certainly resurging where investment stops, as well as in times of humanitarian conflict and during public health emergencies like the COVID-19 pandemic.
Since 2000, global partnership and investment has halved malaria death rates and saved 10.6 million lives, yet half the world is still at risk from the disease, with children under the age of five most vulnerable. In just over two decades, 39 countries and territories have managed to rid themselves of malaria; the most recent being China and El Salvador.
These successes demonstrate that existing tools can achieve local elimination, but the battle is becoming harder, influenced by environmental factors, such as climate, human behaviour, and historic interventions. All of which have a knock-on effect on the mosquitoes that spread this disease, that evolve and adapt to counter our efforts.
In response, we too have to constantly adapt and respond with better tools and strategies. Reducing the disease burden of malaria, from both a public health and economic perspective, is complex and requires tailored solutions, effective use of resources and long-term partnerships and commitment.
Large scale prevention
Each country faced with malaria-endemicity must take a unique, context-specific approach to elimination of the disease and achieving universal health coverage to save thousands of lives. In countries affected by the highest burden of malaria, like Nigeria, large scale operations that achieve high coverage as quickly as possible are critical. Malaria prevention is the first step in lowering the cost of malaria to lives and health systems. Large-scale programmes like seasonal malaria chemoprevention (SMC), which reached 44 million children under five years-old in 2021 through the collective efforts of SMC Alliance organisations, protect those most vulnerable to the disease. Malaria Consortium reached over 20 million of those children and our SMC research has also improved understanding of how people access healthcare services across the areas covered. Without these high coverage interventions, we cannot make progress towards achieving malaria burden reduction and elimination.
Digital solutions
The African continent has primarily been dependent on preventive measures such as LLINs, indoor residual spraying (IRS) and chemoprevention (SMC, intermittent preventive treatment in infants, and intermittent preventive treatment in pregnancy). All these combined have saved many lives but they have not been enough to drive cases down towards the levels of pre-elimination and ultimately, elimination.
Large proportions of populations in low- and middle-income, malaria-endemic countries do not have easy or equitable access to healthcare. Digital health platforms, like the Malaria Consortium-supported upSCALE in Mozambique, are helping to overcome this problem by enabling health workers in local communities to provide diagnosis, treatment and referrals for malaria, as well as logging stock levels of drugs and equipment. This has also helped to lessen the impact of the COVID-19 pandemic.


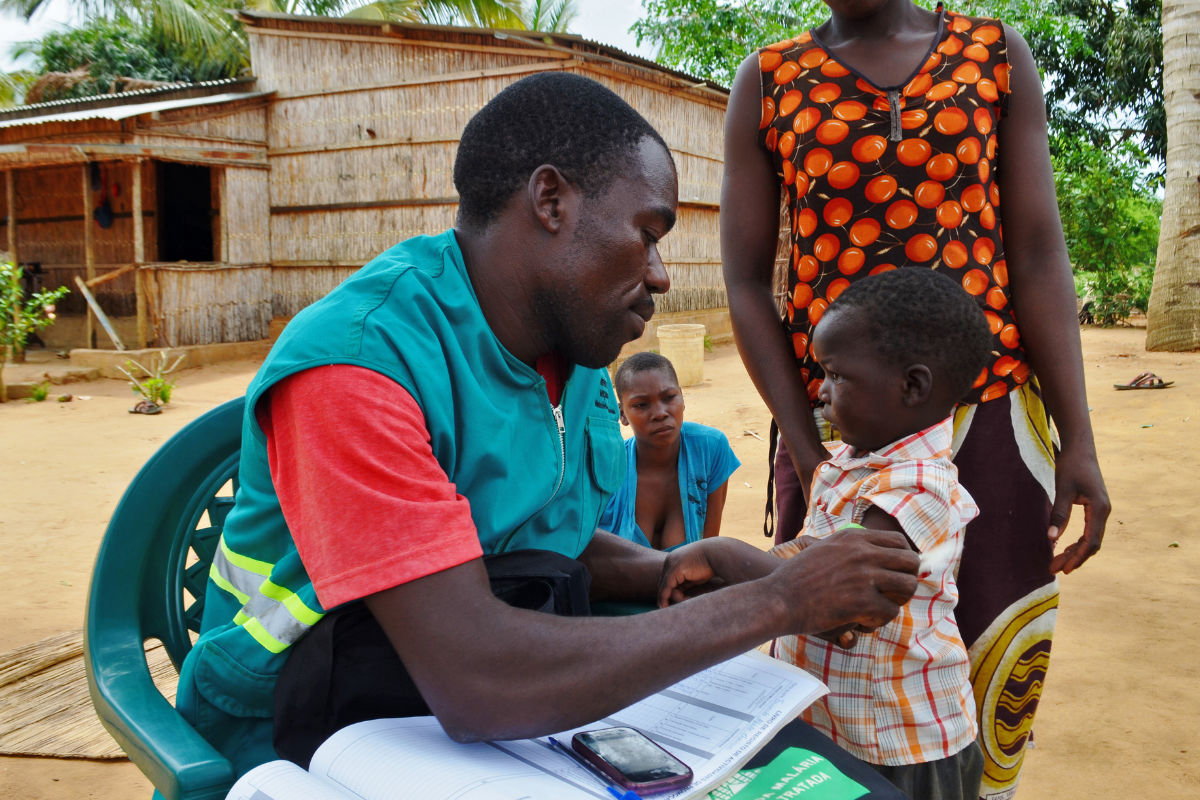
Community ownership and leadership
Community health workers are key to delivering malaria interventions, diagnosing, and treating members of their community and engaging them in prevention measures. They are local people, trained to provide malaria services, free of charge. This allows people who are most susceptible to contracting malaria to receive quality services with far greater ease of access, less economic burden, and without needing travel several hours to a hospital.


Last year, we trained over 40,000 community health workers in malaria diagnosis, understanding that they are often the first point of contact for those suffering illness. To eliminate malaria, community ownership and leadership is crucial and we engage community members directly so that their voices and actions help to secure sustainable change. Watch our animation below to learn why community health workers are vital for improving health outcomes in rural areas.
Surveillance and response
When it comes to meeting the challenge of reaching malaria elimination, robust data collection is also key. More effective and integrated surveillance systems can ultimately not only improve outcomes for malaria but improve health outcomes more widely and build more resilient health systems better able to support public health emergencies like the COVID-19 pandemic.
Malaria Consortium works closely with governments in low-and middle-income countries to strengthen infrastructure and capacity for surveillance within existing health systems and is looking at ways to improve data visualisation trends to make it easier for decision makers to understand and act on data. We also co-chair the RBM Partnership to End Malaria’s Monitoring and Evaluation Working Group whose purpose is to facilitate alignment of partners on strategies and best practices for developing effective systems to monitor and evaluate M&E malaria control programmes.
Incorporating the malaria vaccine
The recommendation by the World Health Organization last year that the RTS,S malaria vaccine should be provided to reduce malaria disease and burden in children living in sub-Saharan Africa is a huge milestone. After thirty years in development, for the first time in history, we are within touching distance of a malaria vaccine being routinely distributed.
There is still work to be done to secure new financing and strengthening health systems to ensure that it does become possible for the RTS,S vaccine to be rolled out globally. The vaccine should be seen as a new and complementary tool alongside the existing combination of interventions that are essential to preventing the devastating effects of malaria: long lasting insecticide nets, parasite-
based diagnosis and case management. Combined, this could spell a marked and sustained acceleration along the continuum to malaria elimination.
Zero malaria is within reach for all countries
The progress seen in many countries and WHO’s bolder targets for malaria elimination are encouraging. Whilst reducing the disease burden of malaria, from both a public health and economic perspective, is complex and requires tailored solutions, zero malaria is within reach of all countries through effective use of resources and long-term partnerships and commitment. The success and rapid expansion of quality services can dramatically reduce the malaria burden, through which the goal of preventing the spread of malaria-resistant parasites can be realised by all countries. Adaptation and responsiveness must be placed at the core of community-delivered models.
Find out more about the impacts of malaria and the projects that are implementing life-saving solutions.
