Universal healthcare is a vital part of breaking free from COVID-19 but gender equity must be at its core
This is a guest post from Alice Tilton, Technical Advisor at Options – an international development consultancy delivering innovative solutions to some of the world’s most complex health challenges.

I recently joined hundreds of other people for the online launch of the World Health Organisations’ (WHO) position paper on ‘Building health systems resilience for universal health coverage and health security during the COVID-19 pandemic and beyond’.
The paper acknowledges that COVID-19 has ‘exacerbated pre-existing health and socioeconomic inequalities within societies’ and calls for a renewed focus on improving and expanding Universal Health Coverage (UHC) to ensure that ‘all people have access to the health services they need, when and wherever they need them, without financial hardship.’
UHC has equity at its heart – equity in the sense that everyone is included, health services are allocated on a need’s basis, and financial contributions are based on ability to pay.
Financial equity is important. We know that poverty is associated with poor health. Indeed, one of the most unfair characteristics of this pandemic is that poorer people are often more exposed (e.g. due to overcrowding), face a higher risk of death (e.g. due to co-morbidities) and they also tend to be more affected by containment measures (e.g. loss of income due to roles in the informal sector or service industry) that aim to stop the spread of the virus.
And the vicious cycle continues: poverty leads to poor health, and poor health leads to poverty. This is a huge worry given the economic impact of COVID-19 is likely to be long-lasting.
In fact, for the first time in 20 years, poverty is likely to significantly increase. The World Bank estimates that between June 2020 to January 2021 there were between 119 and 124 million additional people living in poverty globally. This will have a consequent impact on health.
But while the WHO paper acknowledges the fundamental right to essential health care services and recognises the need for financial protection systems to support this, one particular word was notably absent from the paper: gender.
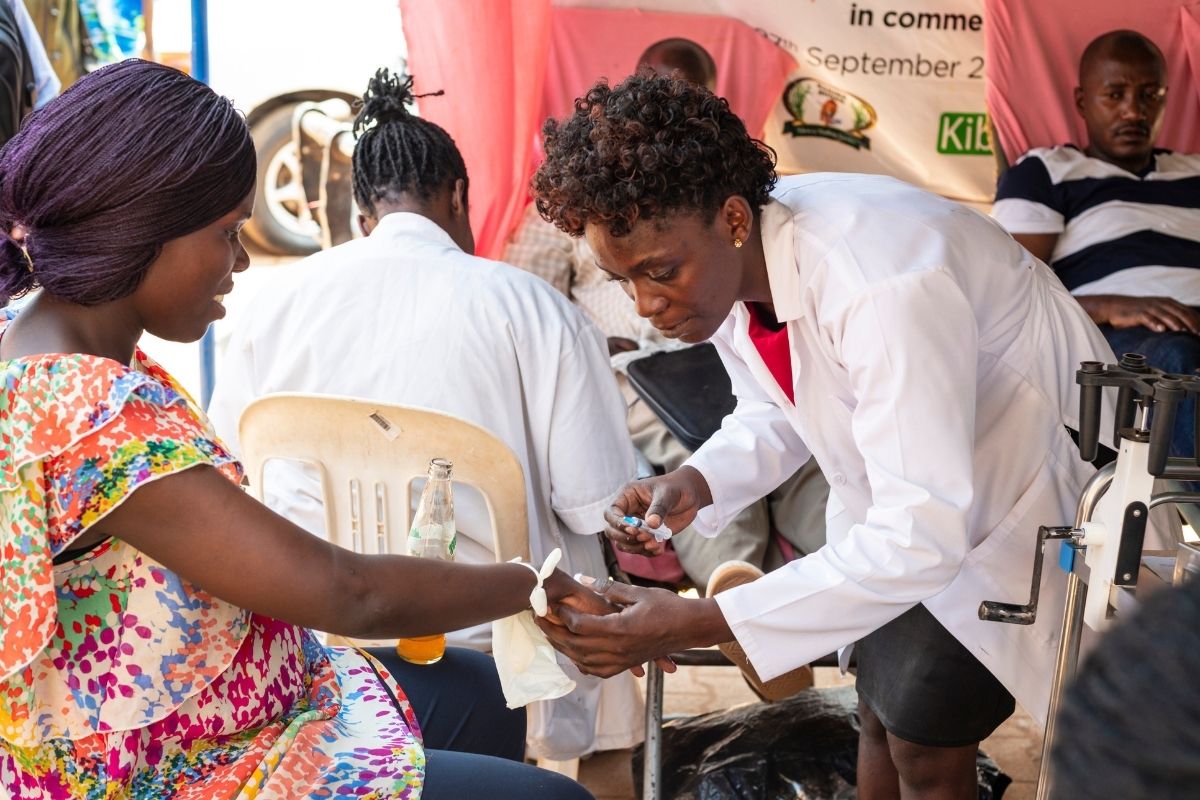
Gender norms affect all our lives. From other research we know that women (particularly those with intersecting identities e.g. race, ethnicity, age, sexuality, disability, etc.) don’t just face financial barriers to accessing healthcare. They can also face higher levels of unpaid care work, unequal power relations and limited decision-making over household resources and their own healthcare, amongst many others.
The principle of equity that underpins UHC must proactively and deliberately include gender equity if we want to make our health systems more resilient to future health emergencies.
How the COVID-10 pandemic affected women and mothers seeking healthcare in Nigeria
At Options, we recently conducted a study on ‘The impact of COVID-19 on maternal and neonatal health in three states in Nigeria’ (Bauchi, Niger, and Lagos).. We identified how maternal and neonatal health (MNH) service delivery, utilisation and outcomes were affected by the pandemic.
We analysed indicators such as antenatal care (ANC) attendance, post-natal care attendance, and maternal, stillbirth, and perinatal mortality from 2017 to 2020. These data were triangulated with interviews with women who had both chosen to and chosen not to visit health facilities during the pandemic as well as interviews with health care workers.
Despite some variation between the three states, all saw a reduction in ANC attendance and deliveries with skilled birth attendants. In interviews with these women, we tried to uncover some of the reasons behind this.
Across all three states, we found that more limited financial resources were one of the main barriers to accessing care, both in terms of costs that might occur at the facility (e.g. medication) and transportation to the facility.
Other barriers included fear of contracting COVID-19, movement restrictions, and socio-cultural gender norms that can restrict women to receiving care only from traditional birth attendants or female members of their family, sometimes with fatal consequences for the mother and baby.
UHC means that all people have access to the health services they need, when and wherever they need them, without financial hardship. Is this enough? For some women, yes. But for others, more needs to be done overcome gender norms that restrict women’s access to healthcare services – even when they’re free.

How can we strengthen gender equity within universal health care?
Socio-cultural gender norms affect numerous areas of all our lives. Intersectional gender equity needs to be embedded within UHC to ensure that people of all genders and intersecting identities can access the healthcare they need.
For example, with regards to women’s access to maternal and neonatal health services (and, likely, other services), more needs to be done to shift power relations so that women have autonomy over their own bodies and their own healthcare – and the means to act on these decisions. For the poorest, it requires that quality, respectful maternal and child health services are entirely free, including transportation and medication.
For those contributing to health insurance schemes, we must ensure that those schemes are themselves gender equitable in their format as employment-based financing can disadvantage women who tend to move between jobs and unpaid care work, resulting in gaps in coverage.
Lowering the number of COVID-19 cases and increasing vaccination rates are vital to saving lives, but a lot more is needed to overcome the huge challenges the pandemic has highlighted.
By incorporating intersectional gender equity into UHC now, we can help ensure that in future health crises, our health systems and our societies don’t leave those already marginalised at further risk of poverty and poor health.
To paraphrase Arundhati Roy, the tragedy of COVID-19 isn’t new, it’s the wreckage of a system that’s been failing to meet the needs of the most marginalised for years. The pandemic is a chance for us to rethink and break free from the past – it must be our portal between this world and the next. UHC is a fundamental part of this journey, but to be successful, it requires intersectional gender equity to be at its heart.
For more information on the universal health coverage and global health, visit the news and views section.
